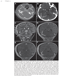
Book Description
In conjunction with the interdisciplinary contributions from a wide variety of health care professionals, Drs. Heather Atkinson, Kim Nixon-Cave, and Sabrina E. Smith aim to provide the necessary tools to effectively treat children with stroke.
The first section reviews the medical fundamentals, covering all major types of strokes. The second section of Pediatric Stroke Rehabilitation focuses on the core of the matter, rehabilitation. The final section expands the understanding of the child’s recovery to the family, community, and school environment.
Select chapters include:
- Personal vignettes written by family members of children who have had a stroke that provides insight into the impact a stroke can have on the child and family
- A family focus box to summarize the main points of the chapter to provide the best tools for caregivers to advocate for their child
- A case study related to the content and family perspective
Pediatric Stroke Rehabilitation also utilizes the World Health Organization’s International Classification of Functioning, Disability, and Health (ICF) framework throughout.
Instructors in educational settings can visit www.efacultylounge.com for additional materials to be used in the classroom.
Pediatric Stroke Rehabilitation: An Interprofessional and Collaborative Approach is an interdisciplinary and invaluable resource for students and clinicians to understand and apply effective evidence-based practice and treatment approaches for childhood stroke. The text will also be of interest to healthcare professionals, specifically physical therapists, occupational therapists, speech-language pathologists, physicians, neuropsychologists, nurses, and educators, who work with children who have experienced a stroke.
More Information
Contents
Dedication
About the Editors
Contributing Authors
Foreword by Rebecca Ichord, MD
Introduction
Section I Pediatric Stroke: Medical Management and the Continuum of Care
Chapter 1 Childhood Arterial Ischemic Stroke
Adam Kirton, MD, MsC, FRCPC
Chapter 2 Perinatal Arterial Ischemic Stroke
Sabrina E. Smith, MD, PhD
Chapter 3 Cerebral Sinovenous Thrombosis in Children
Mubeen F. Rafay, MB.BS, FCPS, MSc
Chapter 4 Intracerebral Hemorrhage in Neonates and Children
Shih-Shan Lang, MD and Gregory G. Heuer, MD, PhD
Chapter 5 The Provision of Rehabilitation Medicine Across the Continuum of Care in PediatricStroke
Phillip R. Bryant, DO
Section II Optimizing Functional Outcomes After Pediatric Stroke
Chapter 6 Examination and Evaluation of Neuromotor Function in Children With Stroke
Heather L. Atkinson, PT, DPT, NCS and Susan V. Duff, EdD, MPT, OTR/L, CHT
Chapter 7 Intervention for Functional Motor Skills in Children With Stroke
Heather L. Atkinson, PT, DPT, NCS; Mardee Greenham, PhD;
Anna Cooper, BOT, GC Paediatric OT; and Anne Gordon, PhD, MSc, BAppSc
Chapter 8 Communication and Feeding in Children With Stroke
Amy Colin, MA, CCC-SLP and Elizabeth Yeh, MA, CCC-SLP
Chapter 9 Cognitive Changes and Potential in Children With Stroke
Amanda Fuentes, PhD, C Psych and Robyn Westmacott, PhD, C Psych, ABPP
Chapter 10 Behavioral and Emotional Functioning in Children With Stroke
Lauren Krivitzky, PhD, ABPP-CN and Danielle Bosenbark, PhD
Section III The Child’s Environment: Family and Community
Introduction
Kim Nixon-Cave, PT, PhD, PCS
Chapter 11 The Family and Child’s Environment in Children With Stroke
Lois J. Robbins, DSW, LSW and Kim Nixon-Cave, PT, PhD, PCS
Chapter 12 Educational Needs of a Child/Adolescent Following a Stroke
Elisa Olson D’Achille, MEd and Juliana Bloom, PhD
Chapter 13 Prevention to Poststroke Rehabilitation: Lifelong Management, Advocacy, and Resources for
Children With Stroke
Kim Nixon-Cave, PT, PhD, PCS and Mary Kay Ballasiotes
Financial Disclosures
Index.
About the Editors
Kim Nixon-Cave, PT, PhD, PCS is physical therapist who specializes in pediatrics. Dr. Nixon-Cave is an associate professor at Thomas Jefferson University, in the role of program director for the entry-level doctor of physical therapy and post-professional education, residency and fellowship education. She practices as a clinician in the Thomas Jefferson University Hospital in pediatrics, primarily the neonatal intensive care unit. Before taking the position at Thomas Jefferson University, Dr. Nixon-Cave was the manager of the Physical Therapy Department in The Center of Rehabilitation Services at The Children’s Hospital of Philadelphia (CHOP) as well as providing direct patient care. She developed a physical therapy Pediatric Residency and Neonatology Fellowship program while at CHOP. Dr. Nixon-Cave has held several faculty appointments, including Temple University, as associate professor, program director and interim chair; associate professor at University of the Sciences; and associate faculty at Arcadia University. She has served on national boards for the American Physical Therapy Association, including the American Board of Physical Therapy Specialties, and American Board of Physical Therapy Residency and Fellowship Education, with the responsibility of developing board certification and post-professional educational programs. She has also focused efforts on addressing the changing health care environment and its impact on delivery of physical therapy services nationally. Recognized by APTA as an Innovator for changes in physical therapy practice as it relates to health care reform, Dr. Nixon-Cave’s clinical focus is developing evidence-based clinical programs and protocols for various patient populations with a specific interest in infants and young children. Quality Improvement Projects have focused on clinical practice, reimbursement, episodic care in inpatient and outpatient practice settings, and best practice guidelines.
Dr. Nixon-Cave is a trained qualitative researcher but participates in research studies that utilize different research approaches including quantitative, qualitative, and mix methodologies to explore and examine health disparities, clinical decision-making of physical therapists, the impact of culture and environment on overall development, and the experience of patients and families and their interaction with the health care system. Dr. Nixon-Cave recently completed a research project examining the current practice of board certified pediatric specialists in physical therapy resulting in a description of specialty practice for physical therapy pediatric certified specialists. Dr. Nixon-Cave has published papers on various topics related to her research area and specifically clinical reasoning and cultural competence in physical therapy.
Dr. Nixon-Cave graduated from the University of Pittsburgh earning her entry-level degree in physical therapy followed by an advanced masters of science degree in Neurologic physical therapy and a PhD in Education from Temple University.
Sabrina E. Smith, MD, PhD is a pediatric neurologist at Kaiser Permanente Oakland Medical Center in Oakland, California. Before moving to Kaiser Permanente, Dr. Smith was a member of the Pediatric Stroke Team at the Children’s Hospital of Philadelphia for 7 years, providing inpatient consultation for newborns and children who experienced a stroke, and running a multidisciplinary outpatient clinic for children who experienced a stroke in the newborn period. Dr. Smith graduated Magna Cum Laude from Princeton University before receiving her MD and a PhD in neurophysiology from New York University School of Medicine. She then completed a residency in pediatrics at the University of California-San Francisco School of Medicine and a residency in pediatric neurology at the University of Pennsylvania School of Medicine and the Children’s Hospital of Philadelphia. Dr. Smith completed a postdoctoral fellowship in cognitive neurology at the University of Pennsylvania School of Medicine where her research focused on the cognitive effects of stroke and other types of brain injury in children. Dr. Smith has published numerous papers on perinatal and childhood stroke and has given talks at national and international meetings.